Simulation exercise helps students focus on interprofessional teamwork

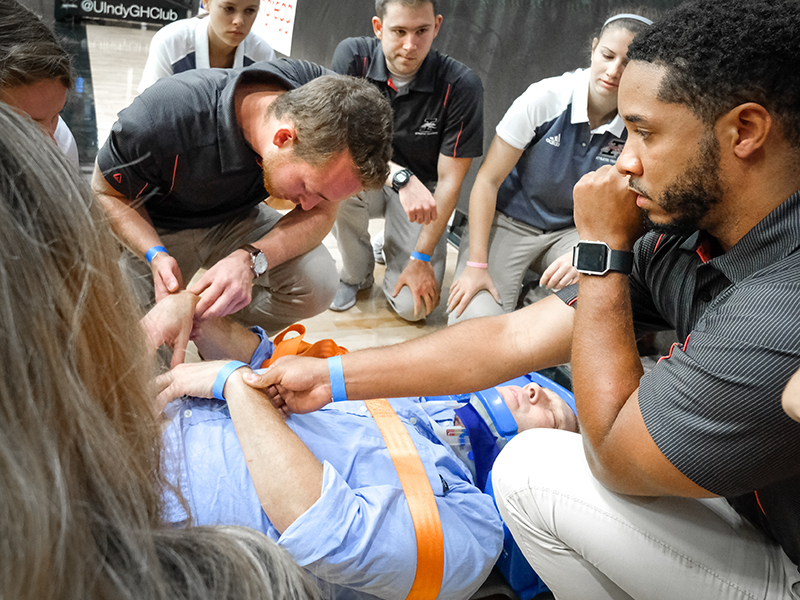
A man suddenly slips and falls in the stands at a basketball game at Nicoson Hall. He groans in pain as concerned onlookers jump to action. Athletic trainers quickly take their places around the patient and begin calling out instructions to protect his spine and head.
The sequence of events that follows–from the ambulance ride to the emergency room to post-trauma care and communication between medical professionals–plays out in a tightly choreographed event as trained health sciences students at the University of Indianapolis participate in a simulated emergency response scenario. The exercise allows the students a “real-life” opportunity to implement the interprofessional and collaborative training that is integral to today’s trending model of healthcare.
“There’s a big push in all of our professions to work more interprofessionally. By giving students the opportunity to do that, that helps them to be more prepared for fieldwork, clinicals or internships,” said Alison Nichols, assistant professor of occupational therapy, one of several faculty members who helped to organize the simulation.
The carefully designed simulation provided students of several disciplines–nursing, physical therapy, occupational therapy, athletic training, psychology and social work–a chance to collaborate at all levels of an emergency scenario. In this case, the patient simulated a serious injury at a campus event and was transported from Nicoson Hall to the UIndy Health Pavilion before being treated in the UIndy Simulation Center. Students coordinated the entire emergency response and treatment plan.
“I was amazed at how important it was for us to speak with each other and to know what each other was doing at all times. By communicating with each other, we could avoid repetition and streamline things for the patient,” said Mimi Chase ’19, a graduate student in social work.
That collaboration is an integral part of the unique and innovative partnership between Community Health Network and the University. Through an interprofessional and team-based approach to learning, students enter the workforce with beneficial experience of collaborating with a variety of healthcare specialities to best meet the patient’s needs amid an increasingly complex healthcare system.
“You are teaching students to look outside the boxes of their professions and look at the other members of the team so that they understand each other’s roles,” said Gurinder Hohl, director, UIndy-Community Health Network partnership.
Hohl explained how that philosophy can impact patient outcomes in a medical setting. Both from the patient and provider perspectives, it’s in everyone’s best interest to reduce hospital readmissions, she said. Effective communication across disciplines helps to improve that workflow.
“When a team is patient-centered, the added impact is that the patients manage their health better because they have resources that have been arranged for them,” Hohl said. “If you don’t have that team-based handover, there are lost opportunities for patient care.”
Paige Buddenhagen ’19 and Jamal Edwards ’19, athletic training, worked on the patient in Nicoson before the ambulance arrived. Edwards was responsible for the patient’s head, which involved calling out instructions to his colleagues as they loaded the patient onto a spine board to avoid further injury, while Buddenhagen coordinated an ambulance.
“I definitely liked seeing the transition from EMS to nursing and how that all works,” Buddenhagen said. “Recognizing and responding in an efficient manner is critical to the patient’s health.”
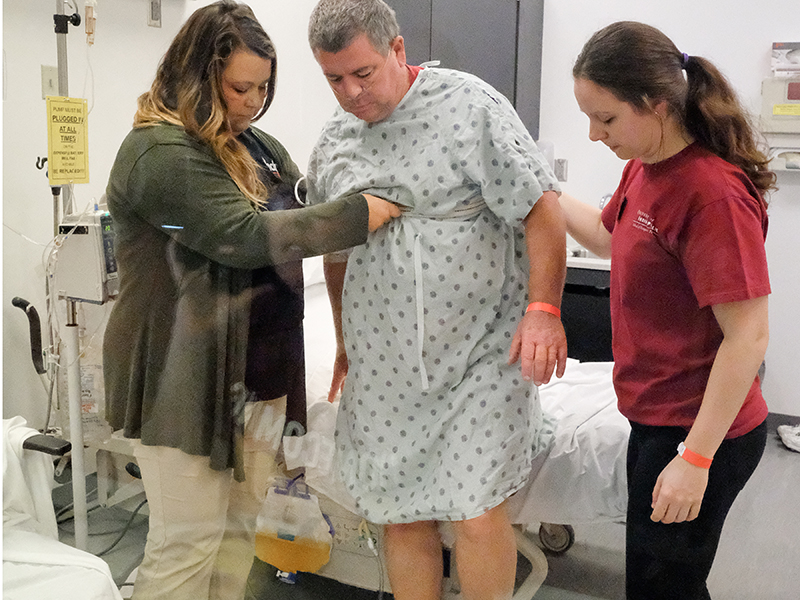
Once the patient was admitted to the hospital, occupational and physical therapy students had the opportunity to collaborate and evaluate the patient’s abilities and needs. Social work and psychology students had new roles to play when alcohol turned up as a factor in the case. Carrie Dettmer ’18, a student in the accelerated nursing program, explained that the team setting gave her confidence.
“When I came upon a situation with substance abuse with this particular simulation patient, I knew that I had the backup of social work and psych coming in behind me,” Dettmer said.
Nurses collaborated with psychologists and social workers to determine the resources available to help the patient with addiction issues.
Michael Craven ’20, clinical psychology doctoral candidate, played the role of staff psychologist at the hospital during the simulation.
“It’s the direction healthcare is going. Being able to have practice, learning what it’s like to work side by side with physical therapists, occupational therapists, social workers, prepares us incredibly to be able to function in that environment,” Craven said.
Written by Sara Galer, Senior Communications Specialist, University of Indianapolis. Contact newsdesk@UIndy.edu with your campus news.